What Is Plantar Fibromatosis?
Plantar fibromatosis, also known as Ledderhose disease, is a benign but potentially progressive condition in which firm, fibrous nodules develop within the plantar fascia — the thick band of connective tissue that runs along the bottom of your foot from the heel to the toes. These nodules, called plantar fibromas, form within the medial band of the plantar fascia and can appear as a single mass or in clusters within the arch of the foot.
While plantar fibromas are non-cancerous, they are often slow-growing and can become increasingly painful during walking and daily activity. They carry a high recurrence rate when not properly managed by an experienced specialist. Left untreated or mismanaged, plantar fibromatosis can significantly impact your quality of life — and in some cases, may mask more serious underlying conditions that require urgent medical evaluation.
Plantar fibromatosis is more common in adults over the age of 40, occurs more frequently in men, and has a higher incidence in individuals of Northern European descent. The condition has a known genetic component and tends to run in families. In approximately 10% of cases, patients also develop similar fibrous nodules in the palms of their hands, a condition known as Dupuytren’s Contracture, which reflects a shared fibroblastic origin between the two conditions.
What Causes Plantar Fibromatosis?
The exact cause of plantar fibromatosis is not always identifiable, and in many cases the condition is multifactorial. Current research points to a combination of genetic predisposition, repetitive microtrauma to the foot, and systemic health factors as the primary drivers.
Genetic predisposition plays a significant role. Plantar fibromatosis belongs to a family of disorders called fibromatoses, which are characterized by abnormal proliferation of fibrous connective tissue. Mutations in the WNT/beta-catenin signaling pathway have been implicated in research. Repetitive stress and microtrauma to the plantar fascia from athletic activity, prolonged standing on hard surfaces, or poorly fitting footwear can also trigger fibroma formation in susceptible individuals.
Certain medications have been associated with plantar fibromatosis, including long-term use of phenytoin (Dilantin), beta-blockers, and some glucosamine supplements. Systemic conditions such as diabetes mellitus, epilepsy, chronic liver disease, and thyroid disorders have also been linked to higher rates of the condition. Understanding these contributing factors is part of a thorough specialist evaluation and helps guide the most appropriate treatment plan for each individual patient.
Symptoms of Plantar Fibromatosis
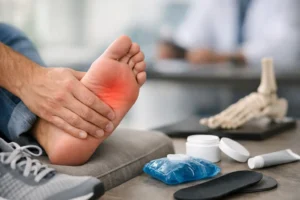
The most common presenting symptom of plantar fibromatosis is a palpable, firm nodule in the arch of the foot. The mass is typically fixed to the plantar fascia and does not move freely when touched. There may be one nodule or several, and the condition can affect one or both feet. Patients commonly experience localized pain or tenderness when walking barefoot, wearing thin-soled shoes, or engaging in prolonged weight-bearing activity. The nodule tends to grow gradually over months to years, and discomfort typically worsens as the mass enlarges. In advanced cases, the fibroma can cause toe contracture or restrict overall foot flexibility, further limiting mobility and quality of life.
How Is Plantar Fibromatosis Diagnosed?
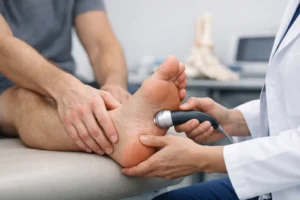
Diagnosis of plantar fibromatosis begins with a thorough clinical examination by a board-certified foot and ankle specialist. The nodule’s characteristic location within the plantar fascia, its firm texture, and its fixed nature are hallmark findings that an experienced clinician will recognize during examination.
Diagnostic imaging plays an important confirmatory role, particularly when the diagnosis is uncertain or surgical planning is required. Ultrasound is a first-line imaging tool that can reveal the characteristic hypoechoic fusiform masses within the plantar fascia and confirm their extent. MRI is the gold standard for soft tissue characterization and is essential when malignancy cannot be excluded based on clinical examination alone. On MRI, plantar fibromas typically appear hypointense on both T1 and T2 sequences — a pattern that helps distinguish them from more aggressive soft tissue lesions.
It is important to understand that biopsy is generally not recommended as a primary diagnostic tool for plantar fibromatosis. Needle biopsy or incisional biopsy can stimulate fibroma growth and significantly increase the risk of recurrence. A definitive histopathologic diagnosis is typically obtained only from surgically excised specimens that are then evaluated by a pathologist.
Why You Should Not Ignore a Mass in Your Foot Arch
One of the most important reasons to seek specialist evaluation for any firm mass in the arch of your foot is that not every plantar nodule is a benign fibroma. Several aggressive and potentially life-threatening conditions can present with symptoms that are nearly identical to plantar fibromatosis. Without proper imaging and specialist evaluation, these diagnoses can be missed — sometimes for months — with serious consequences.
Soft tissue sarcomas, including synovial sarcoma, fibrosarcoma, and epithelioid sarcoma, can arise in the foot and be mistaken for a benign fibroma. These are malignant tumors that require urgent surgical excision with wide margins and may require radiation therapy or chemotherapy. A delay in diagnosis significantly worsens surgical outcomes and, in some cases, survival. Plantar fibrosarcoma is a rare but aggressive malignant variant that can arise directly within the plantar fascia and is clinically indistinguishable from a benign fibroma without imaging and expert evaluation.
Desmoid tumors, also called aggressive fibromatosis, are locally aggressive lesions that do not typically metastasize but carry a high recurrence rate and can invade surrounding nerves, blood vessels, and bone if not properly managed. The foot is also a documented, though rare, site of metastasis from primary cancers including lung, breast, colon, and renal cell carcinoma. An unassuming arch mass can, in some cases, be an early sign of systemic disease. Pigmented villonodular synovitis, tenosynovial giant cell tumors, and peripheral nerve sheath tumors are additional conditions that can mimic plantar fibromatosis and require specialist evaluation to exclude.
A board-certified foot and ankle specialist with access to advanced diagnostic imaging and surgical expertise is the only professional fully equipped to differentiate these conditions, deliver an accurate diagnosis, and ensure you receive the correct treatment from the outset.
The Cost of Delayed or Inadequate Care
Many patients with plantar fibromatosis delay seeking specialist care, attempt to self-treat, or receive generalist advice that is not appropriate for their specific presentation. These approaches consistently lead to poor outcomes. Simple excision of the fibroma nodule alone, without addressing the surrounding plantar fascia, results in recurrence rates that exceed 60 to 100 percent. Without imaging and specialist evaluation, a sarcoma or aggressive fibromatosis can go undetected for months, dramatically worsening surgical outcomes. Untreated fibromas alter gait mechanics over time, creating compensatory patterns that lead to secondary knee, hip, and lower back pain. These compounding problems become their own chronic conditions and can be far more difficult to reverse than the original foot condition.
Early intervention by a qualified specialist leads to better outcomes, simpler treatment courses, and faster recovery. Every week of delay allows a growing fibroma to become harder to treat effectively.
Modern Treatment Options for Plantar Fibromatosis
Treatment for plantar fibromatosis is individualized based on nodule size, symptom severity, rate of growth, and each patient’s activity level and goals. At Family Foot and Leg Center, PA, we take a stepwise, evidence-based approach that prioritizes the least invasive effective option for each patient before considering more aggressive interventions.
Custom functional foot orthotics are the cornerstone of first-line treatment. They reduce tensile load on the plantar fascia, redistribute plantar pressure away from the fibroma, and in some cases may slow or partially arrest fibroma growth. Accommodative padding provides additional symptomatic relief during daily activity and is appropriate for asymptomatic or mildly symptomatic lesions.
Topical verapamil, a calcium channel blocker applied directly to the fibroma, has shown promise in early-stage lesions by inhibiting fibroblast proliferation. Intralesional corticosteroid injections can reduce localized pain and soften the mass, though they do not eliminate the fibroma and serve best as adjunctive therapy alongside other treatments.
Collagenase Clostridium Histolyticum (CCH) injections are FDA-approved for Dupuytren’s contracture and are currently being studied in plantar fibromatosis with promising early clinical results. The enzyme disrupts the collagen matrix of the fibroma, leading to softening and measurable size reduction. This emerging therapy is available at select specialist centers.
Low-dose external beam radiotherapy, typically delivered at 30 to 36 Gy in fractionated doses, is a well-established and evidence-supported non-surgical treatment for plantar fibromatosis. It is particularly effective for painful or growing lesions in patients who wish to avoid surgery. Multiple peer-reviewed studies have demonstrated meaningful pain reduction and stabilization of lesion growth with this approach. Best results are achieved when lesions are under 3 centimeters and treatment is initiated in the early stages of the condition. This option requires coordination between your foot specialist and a radiation oncologist.
Image-guided percutaneous cryoablation is a minimally invasive technique that uses extreme cold delivered through a small probe to destroy fibroma tissue without open surgery. This approach is gaining clinical traction for patients who want an alternative to traditional surgical excision and requires a specialist experienced in soft tissue ablation.
Surgical excision with total or near-total plantar fasciectomy is reserved for refractory, large, or rapidly growing lesions that have not responded to conservative management. Effective surgery requires wide excision that includes most or all of the affected plantar fascia to minimize the risk of recurrence. Simple nodulectomy — removal of the mass alone without the surrounding fascia — carries recurrence rates of 60 to 100 percent and is generally not recommended as a standalone procedure. Following surgery, custom functional foot orthotics are mandatory to accommodate the structural changes that result from fascia removal, and physical therapy is recommended to support gait rehabilitation and return to full activity.
Why Choose Family Foot and Leg Center, PA
At Family Foot and Leg Center, PA, our board-certified foot and ankle surgeons have extensive experience evaluating and treating plantar fibromatosis and complex soft tissue conditions of the foot and ankle. We offer on-site digital X-ray and diagnostic ultrasound, custom orthotics fabrication, and both conservative and surgical treatment pathways — all under one roof. We serve patients throughout Southwest Florida including Naples, Bonita Springs, Cape Coral, Fort Myers, and surrounding communities. Our specialists take the time to evaluate each patient thoroughly, order appropriate imaging when indicated, and develop a treatment plan that reflects the latest evidence-based medicine.
Do not allow a mass in your foot to go unevaluated. Whether your fibroma is newly discovered or has been growing for years, an expert opinion gives you the clarity, accurate diagnosis, and effective care plan you deserve.
Schedule an Appointment with Our Plantar Fibromatosis Specialists
If you have noticed a firm nodule in the arch of your foot, are experiencing pain while walking, or have already been told you have a plantar fibroma and want a specialist’s opinion on your treatment options, contact Family Foot and Leg Center, PA today. Our team is ready to evaluate your condition, provide advanced imaging when needed, and walk you through every available treatment option.
Call us at 239-430-3668 (FOOT) or request an appointment online. We have multiple locations throughout Southwest Florida to serve you conveniently. Early evaluation is the most important step you can take for your foot health — do not wait.
References
Family Foot and Leg Center, PA — Podiatrist Naples FL | Foot Surgery | Heel Pain | Bunion Treatment | Diabetic Foot Care | Sports Podiatry | Serving Marco Island, Naples, Bonita Springs, Fort Myers, Cape Coral, Port Charlotte & Sarasota.
Copyright © 2024 Family Foot & Leg center, P.A. All Rights Reserved.