We are thrilled to share Dr. Singh’s latest article on how Parkinson’s disease impacts foot health and what we can do at ground level to restore mobility! From managing shuffling gaits to custom orthotics, we are dedicated to helping our Port Charlotte community take every step with confidence and safety.
Dr. Sahiba Singh, DPM, AACFAS
Dr. Kevin Lam, DPM, FACFAS

By the time many of my patients walk – or perhaps more accurately, shuffle – into our Family Foot & Leg Center clinic here in Port Charlotte, they aren’t typically focused on their neurological chemical. They aren’t thinking about why their favorite walking shoes suddenly feel like lead weights or why a simple trip to the mailbox has started to feel like navigating a minefield.
As a podiatrist, I occupy a small but vital corner in the multidisciplinary care of people living with Parkinson’s disease. While the world widely recognized world recognizes Parkinson’s for its tremors and facial masking, its impact on the lower limbs is often the “silent’ thief of independence. For many of my patients in Southwest Florida, it is foot pain, a loss of balance, or a sudden, terrifying fall that first disrupts their daily life in a tangible way.
The Foundation of Movement
Parkinson’s is a progressive neurological disorder, but from my chair, it is a mechanical challenge. Walking is a complex symphony; every step requires precise timing, joint flexibility, and sensory feedback. When Parkinson’s interferes with these signals, the “music” of a patient’s gait becomes discordant. In my practice, I see the distinctive ways this condition manifests “at ground level”:
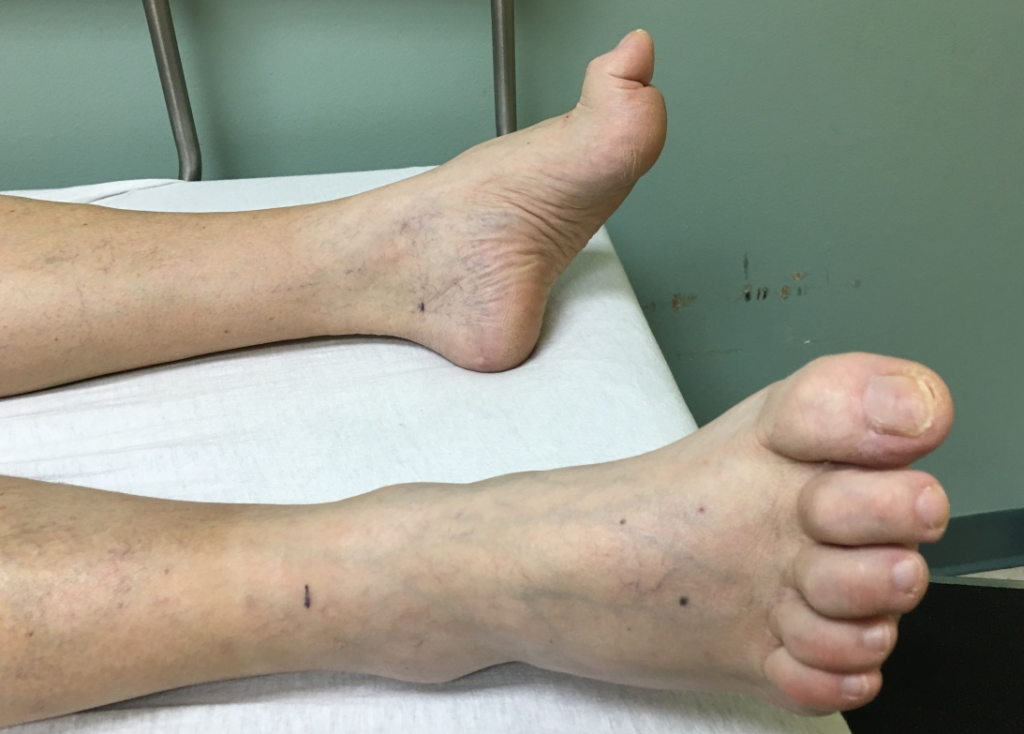
- The Shuffling Gait: This is perhaps the most hallmark pattern. Patients take small, hesitant steps where the heel may barely strike the ground. This shortened stride isn’t just a balance reflex; it shifts immense pressure to the forefoot, leading to painful calluses, metatarsalgia (pain in the ball of the foot), and skin breakdown.
- Freezing of Gait (FOG): This is the sensation of being “glued” to the floor. When a patient wants to move but cannot initiate that first step, their center of gravity often shifts unpredictably. In a town like Port Charlotte, where we value our active lifestyles, this hesitation is a major precursor to falls.
- Dystonia and Toe Curling: Rigidity isn’t limited to the arms. I frequently treat patients whose toes involuntarily curl or “claw.” This makes standard footwear incredibly uncomfortable and leads to secondary issues like corns, ulcers, or painful nail trauma.
Beyond the Tremor: Podiatric Concerns
We often underestimate how much sensory information our feet provide. The soles of our feet are rich in receptors that tell the brain where we are in space. When Parkinson’s slows down the brain’s ability to process this data, even a minor irregularity – a loose rug in the hallway or a slightly uneven sidewalk – becomes a hazard.
Furthermore, the “non-motor” symptoms of Parkinson’s play a role in foot health. Tremors and reduced manual dexterity make basic self-care, like trimming toenails, nearly impossible to do safely. This often results in thickened or ingrown nails that, if left untreated, can cause infections or further alter the way a patient walks to avoid pain.
The Overworked Anchor: Achilles Tendonitis
The Achilles tendon is the largest and strongest tendon in the body, but it isn’t invincible. It absorbs forces up to 12 times your body weight during running. Achilles tendonitis occurs when this tendon becomes irritated through repetitive stress or sudden increases in intensity.
- The Danger Zone: If you ignore a dull ache at the back of your leg, you risk developing tendinosis (chronic degeneration) or, worse, a full rupture.
- Treatment: We emphasize the “10% Rule” – never increase your training volume by more than 10% per week. In the clinic, we may use Shockwave Therapy or physical therapy to stimulate healing in the tendon fibers.
How We Step Forward: Treatment and Strategy
At the Family Foot & Leg Center, our goal is to keep you moving safely. We don’t just look at the foot; we look at the person and their enviroment.
Here are some of the key interventions we focus on:

- Footwear Education: This is one of the simplest yet most powerful tools. I recommend shoes that are lightweight but have a firm heel counter and a non-slip sole. For those struggling with dexterity, we look at Velcro fastenings or elastic laces to maintain independence.
- Custom Orthoses: We often prescribe custom orthotics to redistribute pressure away from the ball of the foot and provide a more stable “platform” for the body.
- Medical Pedicures and Nail Care: Regular professional maintenance prevents the small problems (like an ingrown nail) from becoming big problems (like a fall-inducing gait change).
- Medication Synchronization: I always encourage my patients to schedule their podiatry appointments during their “on” periods – when their dopaminergic medication is at its peak effectiveness. This allows us to see their best possible movement and ensures they are comfortable during the exam.
A message to My Port Charlotte Neighbors
What has struck me most over the years is the psychological weight of foot problems. When walking becomes uncertain, confidence erodes. I see patients withdraw from social groups or stop visiting the Harborwalk because they are afraid of falling.
By addressing foot pain or instability, we aren’t just treating a limb; we are restoring autonomy. We are helping you reclaim the ability to go to the grocery store, visit your grandkids, or simply move around your home without fear.
Parkinson’s is a journey into the unknown, but you don’t have to walk it alone. In our clinic, success is measured in millimeters of stride length and moments of regained balance. Mobility begins where the body meets the ground, and sometimes, preserving your dignity starts with a single, steadier step.
If you or a loved one has Parkinson’s Disease, contact Dr. Singh’s office at (239) 430-3668 or visit www.NaplesPodiatrist.com to schedule an appointment.
Serving Southwest Florida Since 2005, Family Foot & Leg Center has multiple convenient locations throughout Collier, Lee, Charlotte, and Sarasota Counties. Offering pediatric to geriatric family care: Ingrown Toenails, Heel Pain, Bunions, Foot / Ankle Arthritis Pain, Plantar Fasciitis, Foot / Ankle Surgery, Custom Orthotics, and Diabetic Wound Care. In office X-rays, ultrasounds, and minor surgical suite exam rooms. Practice powered by EMR and advanced technologies.
Home of the Lam Minimally Invasive No-Scar Bunion Surgery! Come Discover Why Patients Love Our 5-Star Foot & Ankle Care!
For advanced wound management and diabetic wound healing resources, visit:
WoundHealingExperts.com
Same Day Appointments! Easy Online Appointment Scheduling.

 Fax: (239) 692-9436
Fax: (239) 692-9436 Tel: 239-430-3668
Tel: 239-430-3668